The final selection of the humeral head prosthesis is made after the glenoid aspect of the surgery is complete. The trial body is inserted with humeral head prosthesis trials of the appropriate diameter of curvature and different thicknesses until the desired soft tissue balance is achieved: 150 degrees of elevation, 40 degrees of external rotation of the adducted arm with the subscapularis approximated, 50% posterior subluxation of the humeral head on the posterior drawer test, and 60 degrees of internal rotation of the arm elevated in the coronal plane (scarecrow test). Restricted range of motion might require a head prosthesis of lesser thickness or more soft tissue releases.
If more than 50% posterior translation is present or if the shoulder demonstrates a positive ‘drop back’ sign on passive elevation the surgeon can use one or more of three strategies: (1) a thicker humeral head component, (2) an anteriorly eccentric humeral head component or (3) a rotator interval plication.


In all glenohumeral arthroplasties, it is important to check for posterior abutment of the humerus against the back of the glenoid on external rotation and against the inferior glenoid on adduction – we refer to this critical area as “Pooh Corner”. Checking for these two areas of unwanted bone contact should be done both with the trial components in place and also after the final components have been inserted into their definitive positions. It is also important to thoroughly inspect the joint for bits of bone and to irrigate the joint to remove potential substrate for unwanted bone formation.
After the definitive humeral component has been selected, it is assembled securely on the back table – this assures a tight fit of the Morse taper, rather than what can be achieved by impacting the head on the stem after the stem has been placed in the humerus. Assembling the head on an implanted stem runs the risk of incomplete seating or of changing the position of the stem. Impaction grafting is carried out using cancellous bone harvested from the resected humeral head and soaked in a Vancomycin solution during the time between harvest and insertion. Selective graft placement can fine-tune the position of the stem. If the biceps tendon is in need of tenodesis because of fraying or instability, the tenodesis is performed using an in-and-out technique at the time of prosthesis insertion.
Six No. 2 nonabsorbable sutures are placed in secure bone at the anterior humeral neck for later attachment of the subscapularis tendon. Additional graft is inserted, then the prosthesis is press-fit into the prepared proximal end of the humerus. The height, version, and fixation of the humeral component are carefully checked. The lateral edge of the articular surface should lie just below the cut edge of the humeral neck, which we refer to as the ‘berm’. We pay particular attention to the register; that is, the relationship of the humeral to the glenoid articular surface.
Before closure, the wound is thoroughly irrigated with antibiotic-containing saline and inspected for debris. The joint is again put through a full range of motion to verify smoothness and lack of unwanted contact (e.g., between the medial aspect of the humerus and the inferior glenoid or posteriorly). The wound is not drained. After a gram of Vancomycin powder is placed deep in the wound, the subscapularis is repaired securely to the humeral neck. Another gram of Vancomycin powder is placed on the repaired tendon. The wound is closed in layers. We usually use skin staples to create a secure closure that will tolerate immediate postoperative motion.
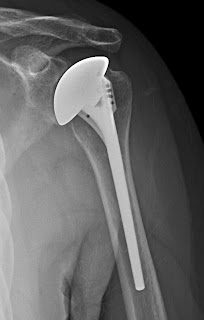
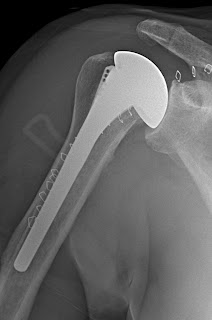
AP and lateral radiographs are obtained in the recovery room to document the immediate postoperative status of the shoulder and to show the patient and family what was done. Films are repeated at six weeks and at two years.



Be sure to click on this link to the Shoulder Arthritis Book.
===
===
Use the "Search" box to the right to find other topics of interest to you.
You may be interested in some of our most visited web pages including:shoulder arthritis, total shoulder, ream and run, reverse total shoulder, CTA arthroplasty, and rotator cuff surgery as well as the 'ream and run essentials'