These authors point out that large glenoid defects pose difficulties in shoulder arthroplasty. They reviewed 44 patients (20 men and 24 women; mean age, 69 years) having a bulk structural graft behind the baseplate of a reverse total shoulder to manage structure defects. The grafts consisted of a humeral head autograft in 29, iliac crest autograft in 1, or femoral head allograft in 14.
These cases used a prosthesis with a bone ingrowth stem on the baseplate
inserted over the bone graft as shown below.
Postoperative scores for the bone graft cohort were significantly lower than those in a cohort without grafting. Complete or partial incorporation was shown radiographically in 81% of grafts.
Six baseplates were considered loose. The major (clinically significant) complication rate was 13.6%. There were 2 graft failures that caused clinical loosening of the baseplate and required revision. Two infections occurred (1 autograft and 1 allograft). One was revised in a 2-stage procedure, and 1 elected to retain the antibiotic spacer. One patient with clinical humeral loosening required revision (autograft). One postoperative dislocation (autograft) occurred. The patient was treated with a closed reduction in the operating room and immobilized for 6 weeks. No further dislocations occurred. Other minor (not clinically significant) complications included 6 patients with scapular notching of grades 1 or 2, and 4 patients with radiolucent lines of 2 mm around the humeral stem but without evidence of gross loosening. This resulted in a total complication rate of 36%.
The baseplate is then screwed into position, assuring that it locks securely in place when tightened.
Secure baseplate and glenosphere fixation was achieved by the method described.
Comment: There is no question that bone deficiency complicates shoulder arthroplasty. The question is when to use a graft and when to work with the bone stock available. That is a decision that can be made only by the operating surgeon based on the glenoid, the prosthesis used and the surgical technique.
We prefer to avoid structural grafts whenever possible because of uncertainty regarding quality, healing, and resistance to resorption. As pointed out in this paper, bone graft failures can cause clinical loosening of the baseplate.
Our preferred method for reverse total shoulder arthroplasty uses a central screw on the baseplate that provides immediate purchase in glenoid cortical bone without having to depend on bone ingrowth into a central peg and that provides lateral offset of the glenosphere to make up for bone deficiency.
In cases of glenoid bone deficiency, we use a small drill to probe the glenoid to find the appropriate area that offers the best bone stock. The depth of solid bone is then verified with the tap: 30 mm is ideal.
The baseplate is then screwed into position, assuring that it locks securely in place when tightened.
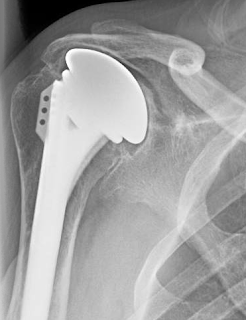
Here is a recent case of failed shoulder hemiarthroplaty with severe glenoid deficiency.
Secure baseplate and glenosphere fixation was achieved by the method described.
This method may be considered instead of bone grafting when there is sufficient remaining bone of quality.
===
Click here to see the new Rotator Cuff Book
Information about shoulder exercises can be found at this link.
Information about shoulder exercises can be found at this link.
Use the "Search" box to the right to find other topics of interest to you.
You may be interested in some of our most visited web pages including:shoulder arthritis, total shoulder, ream and run, reverse total shoulder, CTA arthroplasty, and rotator cuff surgery as well as the 'ream and run essentials'
You may be interested in some of our most visited web pages including:shoulder arthritis, total shoulder, ream and run, reverse total shoulder, CTA arthroplasty, and rotator cuff surgery as well as the 'ream and run essentials'