These authors report on 16 patients undergoing conversion to hemiarthroplasty after failed reverse total shoulder (RSA). All patients had insufficient bone stock for reimplantation of another RSA.
Glenoid loosening was the primary reason for RSA failure in 11 patients. Three required revision surgery because of infection (Propionibacterium, E Coli, Staph Epidermidis).
The case below shows the case of Propionibacterium presenting 8 years (!) after the index procedure. A two stage reconstruction was performed.
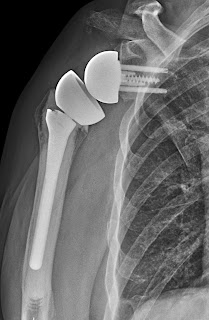
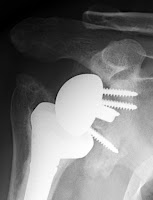
Here is a case of glenoid component failure in a patient with rheumatoid arthritis revised to a hemiarthroplasty. The two year followup show anterosuperior escape.
Postoperative functional outcome for these cases was generally poor at the latest follow-up, with mean Constant, Shoulder Pain and Disability Index, and 11-item version of the Disabilities of the Arm, Shoulder and Hand scores of 25, 37, and 63 points, respectively. Baseline pain also did not improve. Medialization progressed beyond the coracoid in 6 patients, and complete anterosuperior escape was reported in 3 patients. Three postoperative complications were recorded by the final follow-up, including 2 periprosthetic humeral fractures treated conservatively and 1 patient with painful humeral component medialization leading to resection arthroplasty.
Comment: These authors give us some cautionary tales: failed reverse total shoulders can be very difficult to successfully revise, hemiarthroplasty is at best a salvage, and infection is always a consideration - even years after the index surgery. The high incidence of glenoid loosening in this series emphasizes the importance of excellence in glenoid fixation technique and perhaps avoiding RSA when the glenoid bone is of poor quality or quantity. Three cases had scapular fractures, possibly related to weakening of the scapular spine by a superiorly placed screw. The occurrence of periprostheic humeral fractures emphasizes the importance of humeral bone preservation and fixation with impaction grafting rather than cement.
The key seems to be secure fixation of both the glenoid and humeral component with maximal bone preservation on both sides:
To review, there are several important failure modes after reverse total shoulder. Infection is one of the more common and is probably related to the fact that many reverse total shoulders are performed as revisions after multiple prior surgeries coupled with the dead space created when the humerus is displaced distally by the procedure. As with anatomic shoulders, Propionibacterium is a frequently cultured organism from failed reverse total shoulders, which can present with loosening in the absence of the usual clinical signs of infection
The infection with Propionibacterium in the x-ray on the left was treated with a single stage exchange to a long stem prosthesis. The patient is currently asymptomatic six years after the revision.
The infection with Propionibacterium in the x-ray on the left was treated with a single stage exchange to a long stem prosthesis. The patient is currently asymptomatic six years after the revision.
Instability can result from falls, suboptimal component selection, component malposition, bulky tissues in the posterior shoulder, leverage of the humeral component against the glenoid , or lack of sufficient compressive effect by the deltoid.

Early closed reduction can be successful. Recurrent or chronic instability may require surgical revision. The case below shows a failed anatomic prosthesis for fracture with anterosuperior escape that was treated with a reverse that dislocated recurrently.


The prosthesis was revised to a hemiarthroplasty that was unsatisfactory. Finally a successful revision was accomplished by the removal of posterior scar tissue and revision to a reverse with a 40 mm set of components.

Shown below is another example where stability was restored by changing to a larger diameter of curvature and increasing the thickness of the polyethylene and humeral cup.
The risk of humeral fracture is increased in revision surgery, by falls and when the humeral component fixation results in an abrupt transition between a cemented or press fit diaphyseal stem tip and osteopenic bone distal to the prosthetic tip These fractures deserve a trial at closed management.

in that surgical revision can be very complex

Scapular and acromial fractures can result from excessive deltoid tension producing a fatigue fracture or from bone weakened by screw placement. These fractures are preferably treated non-operatively.

Scapular and acromial fractures can result from excessive deltoid tension producing a fatigue fracture or from bone weakened by screw placement. These fractures are preferably treated non-operatively.
Scapular notching is a prominent complication, particularly common in prosthetic designs that medialize the humerus or when the glenoid component is positioned high on the glenoid bone.

The issues with notching are not so much the ‘notch’ in the scapula but the radiographically unseen damage to the polyethylene of the humeral component
and to glenoid component fixation
Notching may also be associated with unwanted bone formation that limits the range of motion
Humeral component failure may result from dissociation of the cup from the stem
Glenoid failure may result from glenosphere-baseplate dissociation,
glenoid fracture,
or failure of fixation
While some cases can be reconstructed, others require salvage conversion to a hemiarthroplasty after glenoid component removal; the clinical results of this conversion are generally poor.
Neurologic lesions can result from dissection, retraction or over lengthening of the arm. Finally, there has been some concern about loss of active external rotation with reverse total designs that medialize the tuberosity, prompting consideration of latissimus dorsi transfers; this problem seems less of an issue with those designs that maintain ‘East-West” tensioning of the residual cuff posteriorly.
----
Use the "Search" box to the right to find other topics of interest to you.
You may be interested in some of our most visited web pages including:shoulder arthritis, total shoulder, ream and run, reverse total shoulder, CTA arthroplasty, and rotator cuff surgery as well as the 'ream and run essentials'
You may be interested in some of our most visited web pages including:shoulder arthritis, total shoulder, ream and run, reverse total shoulder, CTA arthroplasty, and rotator cuff surgery as well as the 'ream and run essentials'






















