These authors have an extensive experience with using reverse total shoulder as a revision procedure, performing143 such cases between 2005 and 2010. 102 patients did not undergo grafting, but in 41 they used bone grafting because of glenoid bone deficiency. 40 of the shoulders had follow-up of more than two years (mean, 3.1 years). 16 had central glenoid defects, 13 had posterior defects, 10 had superior defects and 1 had an inferior defect. The arthroplasty systems used included the Comprehensive Reverse Shoulder (20 shoulders), the Encore Reverse Shoulder Prosthesis (10 shoulders), the Delta III (1 shoulder) Delta Xtend (7 shoulders) and the Aequalis Reversed Shoulder (2 shoulders). Fifteen prostheses had a lateral center of rotation, and twenty-five had a medial center of rotation.
Seven of the 40 patients required another revision surgery because of glenoid loosening (four patients), instability (two patients), or infection (one patient). Of the five structural grafts, one of them failed at 1.2 years secondary to glenoid loosening. The other three failures for glenoid loosening involved cancellous allograft only (two shoulders), or mixed cancellous autograft and allograft (one shoulder).
The two year revision-free survival (76%) and the glenoid radiographic loosening-free survival (89%) were both worse than that for patients who had not required glenoid bone grafting.
Increasing age, revision of a total anatomic or reverse shoulder arthroplasty in contrast to a hemiarthroplasty, and smoking were associated with the need for revision surgery.
Increased rates and grades of glenoid lucency were seen in patients with an increased BMI, a history of total shoulder arthroplasty, an implant with a lateral center of rotation, and in those who smoked.
Comment: The use of a reverse total shoulder in the revision of a failed arthroplasty is known to be among the most challenging applications of this type prosthesis (to whit there were 6 intraoperative humeral fractures in this series). This is a very interesting report in that it indicates the need to individualize the technique when a reverse total shoulder is used to manage a failed joint replacement. In this series five different types of prostheses with three different types of bone graft where used to mange four different types of bone defects after three different types of prior joint replacement (hemiarthroplasty, total shoulder arthroplasty or reverse total shoulder). Once again we see the effect of (1) patient factors (age, BMI, smoking status), (2) shoulder problem characteristics (type of prior arthroplasty, amount and location of the bone defect), and (3) the procedure (type of graft, type of prosthesis). We don't have data on the physician providing the treatment, but that may have had an effect on the survival rate as well.
A major takeaway is that compromised bone quantity and quality can contribute to the risk of glenoid component failure in revision reverse total shoulders: those shoulders needing bone graft, shoulders of smokers and those shoulders that had the removal of a previously placed glenoid component were at greater risk for failure of the reversed glenoid component.
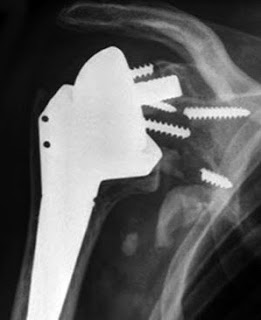
Here's a thought-provoking x-ray, not from this article.
And here's a recent case from our practice - fortunately one without a glenoid bone defect. Note the use of a glenoid component with a long screw for obtaining secure fixation of the glenosphere to the glenoid bone.
=
Increasing age, revision of a total anatomic or reverse shoulder arthroplasty in contrast to a hemiarthroplasty, and smoking were associated with the need for revision surgery.
Increased rates and grades of glenoid lucency were seen in patients with an increased BMI, a history of total shoulder arthroplasty, an implant with a lateral center of rotation, and in those who smoked.
Comment: The use of a reverse total shoulder in the revision of a failed arthroplasty is known to be among the most challenging applications of this type prosthesis (to whit there were 6 intraoperative humeral fractures in this series). This is a very interesting report in that it indicates the need to individualize the technique when a reverse total shoulder is used to manage a failed joint replacement. In this series five different types of prostheses with three different types of bone graft where used to mange four different types of bone defects after three different types of prior joint replacement (hemiarthroplasty, total shoulder arthroplasty or reverse total shoulder). Once again we see the effect of (1) patient factors (age, BMI, smoking status), (2) shoulder problem characteristics (type of prior arthroplasty, amount and location of the bone defect), and (3) the procedure (type of graft, type of prosthesis). We don't have data on the physician providing the treatment, but that may have had an effect on the survival rate as well.
A major takeaway is that compromised bone quantity and quality can contribute to the risk of glenoid component failure in revision reverse total shoulders: those shoulders needing bone graft, shoulders of smokers and those shoulders that had the removal of a previously placed glenoid component were at greater risk for failure of the reversed glenoid component.
Here's a thought-provoking x-ray, not from this article.
And here's a recent case from our practice - fortunately one without a glenoid bone defect. Note the use of a glenoid component with a long screw for obtaining secure fixation of the glenosphere to the glenoid bone.
=
Check out the new Shoulder Arthritis Book - click here.
Use the "Search" box to the right to find other topics of interest to you.
You may be interested in some of our most visited web pages including:shoulder arthritis, total shoulder, ream and run, reverse total shoulder, CTA arthroplasty, and rotator cuff surgery as well as the 'ream and run essentials'