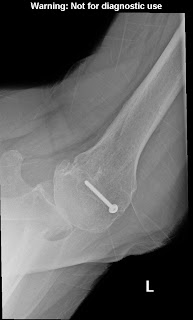
These authors point out that computed tomography scans are often obtained before total shoulder arthroplasty to assess glenoid deformity. There is much current discussion regarding what processing of the CT data is necessary to gain the desired information.
The purpose of this study was to determine whether inclusion of the medial border and inferior angle is necessary for accurate measurement of scapular version, inclination, and humeral subluxation.
They obtained 14 CT scans in patients with B2 type glenoids, measuring glenoid version, inclination, depth, and humeral subluxation on 2-dimensional CT images corrected to the plane of the scapula. The measurements were then repeated in randomized, blinded fashion after subtracting 12.5%, 25%, and 50% of the scapula from the medial border and 12.5%, 25%, and 50% of the scapula from the inferior angle.
They found that measurement of retroversion did not significantly differ between measurement of the full scapula and measurement of any of the incomplete scapulas, with the exception of the subtraction of 50% of the scapular width, which caused retroversion to be overestimated by 4.7° (P = .006) and led to inaccurate measurement of subluxation and glenoid depth.
Comment: In their discussion the authors point out that increased medical imaging is thought to be contributing to the increasing incidence of thyroid cancer and that and CT scans account for almost half of all medial imaging– related radiation.
They obtained 14 CT scans in patients with B2 type glenoids, measuring glenoid version, inclination, depth, and humeral subluxation on 2-dimensional CT images corrected to the plane of the scapula. The measurements were then repeated in randomized, blinded fashion after subtracting 12.5%, 25%, and 50% of the scapula from the medial border and 12.5%, 25%, and 50% of the scapula from the inferior angle.
They found that measurement of retroversion did not significantly differ between measurement of the full scapula and measurement of any of the incomplete scapulas, with the exception of the subtraction of 50% of the scapular width, which caused retroversion to be overestimated by 4.7° (P = .006) and led to inaccurate measurement of subluxation and glenoid depth.
Comment: In their discussion the authors point out that increased medical imaging is thought to be contributing to the increasing incidence of thyroid cancer and that and CT scans account for almost half of all medial imaging– related radiation.
One must question, therefore, whether routine preoperative CT scans provide sufficient additional information over a standardized axillary view to justify the additional cost and radiation exposure. We have yet to find a study that shows that patients receiving preoperative CT scans realize better clinical outcomes than those who do not.
We rarely find that a pre-shoulder arthroplasty CT scan is necessary to understand the pathoanatomy of the arthritic shoulder.
Our approach to preoperative imaging is discussed below
The purpose of imaging of the shoulder is to help establish the diagnosis, to determine the severity of the pathoanatomy, to help in surgical planning, and to enable the surgeon to illustrate the condition of the shoulder for the patient. Unless a specific research protocol is in place, we resist the temptation to ‘over-image’ , i.e. obtaining scans or reconstructions that are not necessary for the care of the patient such as that shown below.
When taken properly, the standardized anteroposterior and axillary views indicate the thickness of the cartilage space between the humerus and the glenoid, the relative positions of the humeral head and the glenoid, the presence of osteophytes, the degree of osteopenia, and the extent of bony deformity and erosion.
Since arthritis usually involves the central aspect of the humeral head,
A third view, the templating view, is obtained when humeral arthroplasty is being considered. This view is an anteroposterior (AP) view of the humerus taken with the arm in 30 degrees of external rotation relative to the x-ray beam with a magnification marker added. This view places the humeral neck in maximal profile and allows a comparison of proximal humeral anatomy with that of various humeral prostheses. In templating, it is important to recognize that the humeral canal is not cylindrical – the medial-lateral dimension is usually wider than the anteroposterior dimension so that the AP view may overestimate the size of the stem that will fit the diaphysis. This view is also useful for determining whether sufficient osteoporosis is present to merit special consideration at the time of arthroplasty
Advanced imaging may be useful in the unusual case where the anatomy is distorted by prior injury or surgery, when there is concern about the amount of bone available for reconstruction, or when the standardized plain films cannot be obtained. In the great majority of cases, however, the extra cost and radiation of the CT scan can be avoided through the use of these standardized plain films. In that we can learn what we need to know about the status of the rotator cuff from physical examination and plain radiographs, shoulder MRIs are rarely needed unless indicated to exclude avascular necrosis or tumor. An MRI of the neck may be useful in evaluating patients suspected of having cervical radiculopathy, myelopathy, stenosis or a syrinx.
Be sure to click on this link to the Shoulder Arthritis Book.
---
Use the "Search" box to the right to find other topics of interest to you.
You may be interested in some of our most visited web pages including:shoulder arthritis, total shoulder, ream and run, reverse total shoulder, CTA arthroplasty, and rotator cuff surgery as well as the 'ream and run essentials'
See from which cities our patients come.
See the countries from which our readers come on this post.
The observation that CT scans may offer a few degrees of increased precision in the measurement of glenoid version does not convince us that this precision improves the quality of the surgery or the clinical outcome. Almost always standardized plain films are sufficient to garner the needed information and, as is shown below, information can be gathered from properly taken plain films that cannot be gathered on CT scans . In that proper radiographic technique (like surgical technique) is necessary to achieve the desired outcome, we take time to assure that our x-ray technologists know what we are seeking in the images.
The first key view is the anteroposterior in the plane of the scapula taken so that the x-ray beam passes through the glenohumeral joint. This view shows the superior-inferior position of the humeral head relative to the glenoid, the presence of osteophytes on the humeral head and glenoid, joint space narrowing, the degree of medial displacement of the humerus in relation to the lateral acromial line, the quality of the humeral and glenoid bone, the presence of loose bodies, and the presence of humeral head collapse or deformity.
The second key view is the axillary view taken with the arm in the functional position of elevation in the plane of the scapula and oriented so that both the spinoglenoid notch and the scapular neck are visible. This view shows a different perspective of the humeral anatomy, the amount of glenoid bone, the shape of the glenoid, its version in relation to the plane of the scapula and the relationship of the humeral head to the glenoid fossa. We have named the axillary view taken in with the arm elevated in the plane of the scapula the ‘truth’ view. This is because it demonstrates the glenohumeral relationships in the functional position of elevation; this is in contrast to CT scans, which have the disadvantage of being taken with the arm in the adducted position
The first key view is the anteroposterior in the plane of the scapula taken so that the x-ray beam passes through the glenohumeral joint. This view shows the superior-inferior position of the humeral head relative to the glenoid, the presence of osteophytes on the humeral head and glenoid, joint space narrowing, the degree of medial displacement of the humerus in relation to the lateral acromial line, the quality of the humeral and glenoid bone, the presence of loose bodies, and the presence of humeral head collapse or deformity.
The second key view is the axillary view taken with the arm in the functional position of elevation in the plane of the scapula and oriented so that both the spinoglenoid notch and the scapular neck are visible. This view shows a different perspective of the humeral anatomy, the amount of glenoid bone, the shape of the glenoid, its version in relation to the plane of the scapula and the relationship of the humeral head to the glenoid fossa. We have named the axillary view taken in with the arm elevated in the plane of the scapula the ‘truth’ view. This is because it demonstrates the glenohumeral relationships in the functional position of elevation; this is in contrast to CT scans, which have the disadvantage of being taken with the arm in the adducted position
Unfortunately, many of the ‘axillary views’ sent to us on patients for consultation are taken without standardization, making it impossible to determine the important features of the glenohumeral joint as shown below.
When taken properly, the standardized anteroposterior and axillary views indicate the thickness of the cartilage space between the humerus and the glenoid, the relative positions of the humeral head and the glenoid, the presence of osteophytes, the degree of osteopenia, and the extent of bony deformity and erosion.
Since arthritis usually involves the central aspect of the humeral head,
joint space narrowing is most evident on the truth view as opposed to images made with the arm at the side. Of even greater importance is the ability of the axillary ‘truth’ view to show posterior subluxation or ‘functional decentering’ that is not evident in images taken with the arm at the side.
The degree of posterior subluxation can be measured as (a) the position of the center of the humeral head in relation to the plane of the scapula, (b) the position of the center of the humeral head in relation to the glenoid face or (c) the point of contact of the humeral articular surface on the glenoid articular surface. We prefer the latter because it is this point of contact that reflects the degree of centering of the net humeral joint reaction force on the glenoid. It is the malcentering of this joint reaction force that leads to posterior instability, posterior glenoid wear and to rocking horse loosening of prosthetic glenoid components. The standardized axillary view also enables the surgeon to see the shape of the glenoid surface. Three main types have been described: concentric wear (type A)
In actual practice, there are so many intermediate types of glenoid pathoanatomy that rigorous separation into a few distinct classes is difficult.
An important aspect of glenoid pathology is the amount of the glenoid that is involved in the pathologic concavity, known as the ‘neoglenoid. Finally, the standardized axillary view enables the measurement of the degree of glenoid retroversion in relation to the body of the scapula. Thus, on the standardized axillary view, the surgeon can usually determine the major important characteristics of glenohumeral arthritic pathoanatomy: the amount of joint space narrowing, the degree of retroversion, the degree of posterior subluxation with the arm in a functional position, the glenoid shape, the percentage of the glenoid involved in the pathologic concavity and the angle of retroversion.
Because of their low cost and freedom from metal artifacts, standardized axillary views provide a practical and reliable way to document the postoperative anatomy sequentially over time and to compare it to what was present before surgery.
A third view, the templating view, is obtained when humeral arthroplasty is being considered. This view is an anteroposterior (AP) view of the humerus taken with the arm in 30 degrees of external rotation relative to the x-ray beam with a magnification marker added. This view places the humeral neck in maximal profile and allows a comparison of proximal humeral anatomy with that of various humeral prostheses. In templating, it is important to recognize that the humeral canal is not cylindrical – the medial-lateral dimension is usually wider than the anteroposterior dimension so that the AP view may overestimate the size of the stem that will fit the diaphysis. This view is also useful for determining whether sufficient osteoporosis is present to merit special consideration at the time of arthroplasty
Advanced imaging may be useful in the unusual case where the anatomy is distorted by prior injury or surgery, when there is concern about the amount of bone available for reconstruction, or when the standardized plain films cannot be obtained. In the great majority of cases, however, the extra cost and radiation of the CT scan can be avoided through the use of these standardized plain films. In that we can learn what we need to know about the status of the rotator cuff from physical examination and plain radiographs, shoulder MRIs are rarely needed unless indicated to exclude avascular necrosis or tumor. An MRI of the neck may be useful in evaluating patients suspected of having cervical radiculopathy, myelopathy, stenosis or a syrinx.
Be sure to click on this link to the Shoulder Arthritis Book.
---
Use the "Search" box to the right to find other topics of interest to you.
You may be interested in some of our most visited web pages including:shoulder arthritis, total shoulder, ream and run, reverse total shoulder, CTA arthroplasty, and rotator cuff surgery as well as the 'ream and run essentials'
See from which cities our patients come.
See the countries from which our readers come on this post.