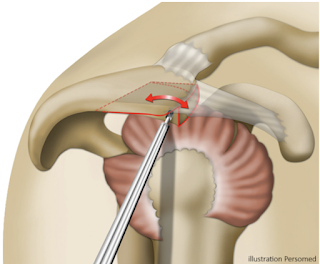
and his x-ray showing the traction spur in the coracoacromial ligament, but - notably - not encroaching on the rotator cuff space

Since this publication, numerous authors have tried to understand if these acromial changes are an effect or a cause of degenerative cuff disease.
The authors of Published Evidence Relevant to the Diagnosis of Impingement Syndrome of the Shoulder pointed out that acromioplasty for impingement syndrome of the shoulder is one of the most common orthopaedic surgical procedures. They sought high levels of evidence in the published literature related to five hypotheses pertinent to the concept of the impingement syndrome and the rationale supporting acromioplasty in its treatment:
(1) clinical signs and tests can reliably differentiate the so-called impingement syndrome from other conditions,
(2) clinically common forms of rotator cuff abnormality are caused by contact with the coracoacromial arch,
(3) contact between the coracoacromial arch and the rotator cuff does not occur in normal shoulders,
(4) spurs seen on the anterior aspect of the acromion extend beyond the coracoacromial ligament and encroach on the underlying rotator cuff, and
(5) successful treatment of the impingement syndrome requires surgical alteration of the acromion and/or coracoacromial arch.
They found that these hypotheses were not supported by high levels of evidence.
Recently, the authors of Arthroscopic Rotator Cuff Repair with and without Acromioplasty in the Treatment of Full-Thickness Rotator Cuff Tears Long-Term Outcomes of a Multicenter, Randomized Controlled Trial provided a longer term followup of their original study: Arthroscopic rotator cuff repair with and without acromioplasty in the treatment of full-thickness rotator cuff tears: a multicenter, randomized controlled trial with the goal of determining the long-term efficacy of subacromial decompression in patients with full-thickness rotator cuff tears.
Eighty-six patients were randomized in the original trial, with 31 of 45 from the group without acromioplasty and 25 of 41 from the acromioplasty group returning for long-term follow-up (mean: 11 years).
There was no significant difference in WORC scores between the groups with and without acromioplasty at the time of the long-term follow-up (p = 0.30).
Seven (16%) of the 45 patients in the group without acromioplasty and one (2%) of the initial 41 patients allocated to acromioplasty underwent or were recommended to have reoperation.

Comment: Two experienced surgeons performed all the surgeries. The distribution of primary cases and the distribution of revision cases between these two surgeons is not presented.
The authors stated, "Tears of ≤4 in size of one or more tendons were included," however the tear sizes in the acromioplasty and non acromioplasty groups are not presented. Furthermore, the initial tear sizes in the revised and unrevised shoulders are not presented. Thus is not clear whether the cuff pathology was worse in the shoulders with type 2 or type 3 acromions.
The integrity of the cuff / retears in the two groups were not routinely evaluated by MRI or ultrasound. The operative findings - particularly the integrity of the cuff and the degree of subacromial scarring- in the revised cases are not presented. Thus the cause of symptoms leading to repeat surgery is not clarified. This study does not provide robust evidence to support the concept that acromioplasty has "a protective effect on the rotator cuff repair in patients with an amorphous acromion."
A few additional thoughts in closing.
....as well as his admonition (p 13), that "the coracoacromial ligament has an important duty [restraining the humeral head] and should not be thoughtlessly divided at any operation."
The articulation between the coracoacromial arch needs - as is the case for any articulation - to be smooth and to provide a broad contact area. As Neer pointed out, acromial spurs arise within the coracoacromial ligament. As such these spurs rarely encroach on the cuff. If there is a prominence to palpation of the curvature of the CA arch (which is uncommon), it can be conservatively smoothed with a bur without transection of the ligament or a major acromial resection.
Finally, some techniques of rotator cuff repair can disrupt the smoothness of the subacromial articulation by adding "top knots" that protrude from the surface of the repaired cuff.



In performing cuff repair, it may be best to position knots so that they do not rub against the CA arch.
You can support cutting edge shoulder research that is leading to better care for patients with shoulder problems, click on this link.
To add this blog to your reading list in Google Chrome, click on the reading list icon
Follow on twitter: https://twitter.com/shoulderarth
Follow on facebook: click on this link
Follow on facebook: https://www.facebook.com/frederick.matsen
Follow on LinkedIn: https://www.linkedin.com/in/rick-matsen-88b1a8133/
Here are some videos that are of shoulder interest
Shoulder arthritis - what you need to know (see this link).
How to x-ray the shoulder (see this link).
The ream and run procedure (see this link).
The total shoulder arthroplasty (see this link).
The cuff tear arthropathy arthroplasty (see this link).
The reverse total shoulder arthroplasty (see this link).
The smooth and move procedure for irreparable rotator cuff tears (see this link).
Shoulder rehabilitation exercises (see this link).