It is helpful to contrast shoulder PJI with PJI of the hip and knee. The organisms most commonly responsible for hip and knee periprosthetic infections are shown below (see Periprosthetic infections)

These infections usually present within days or weeks following the arthroplasty often with the typical symptoms, signs, and laboratory evidence of infection (fever, swelling, tenderness, erythema, elevated white blood cell counts, erythrocyte sedimentation rate, C reactive protein, serum inflammatory markers and positive joint aspirates for cells and bacteria).
The risk of periprosthetic infections (PJI) of hip and knee arthroplasty is increased by poor health, such as morbid obesity, malnutrition, hyperglycemia, uncontrolled diabetes mellitus, rheumatoid arthritis, preoperative anemia, cardiovascular disorders, chronic renal failure, smoking, alcohol abuse and depression (see Patient-related medical risk factors for periprosthetic joint infection of the hip and knee).
The situation is quite different for periprosthetic infections of the shoulder, the great majority of which are caused by Cutibacterium, an organism found on and in healthy skin (see Prognostic factors for bacterial cultures positive for Propionibacterium acnes and other organisms in a large series of revision shoulder arthroplasties performed for stiffness, pain or loosening).
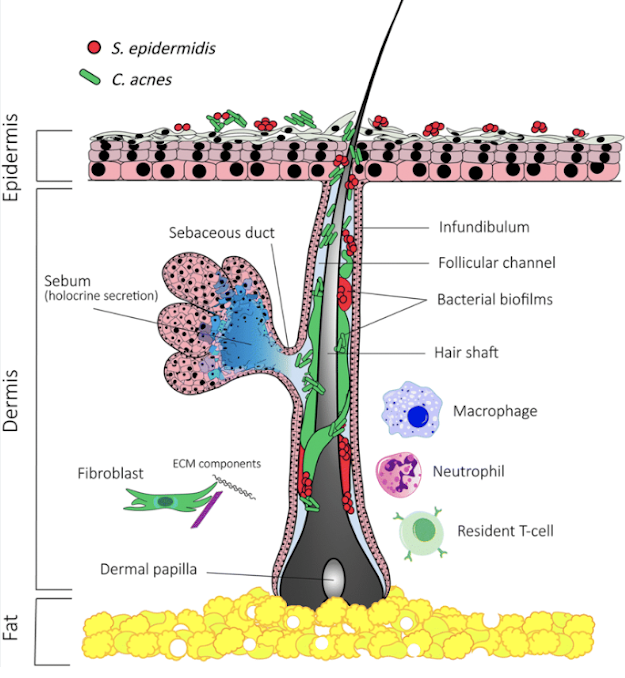
It is recognized that the healthy skin of the chest has abundant dermal pilosebaceous units containing Cutibacterium and that these dermal structures cannot be sterilized by oral or topical treatment (see Origin of propionibacterium in surgical wounds and evidence-based approach for culturing propionibacterium from surgical sites and Cutaneous microbiology of patients having primary shoulder arthroplasty and Propionibacterium persists in the skin despite standard surgical preparation and Propionibacterium can be isolated from deep cultures obtained at primary arthroplasty despite intravenous antimicrobial prophylaxis and Randomized controlled trial of chlorhexidine wash versus benzoyl peroxide soap for home surgical preparation: neither is effective in removing Cutibacterium from the skin of shoulder arthroplasty patients and While home chlorhexidine washes prior to shoulder surgery lower skin loads of most bacteria, they are not effective against Cutibacterium (Propionibacterium)). These structures are inevitably incised during the deltopectoral incision, allowing the bacterium to inoculate the arthroplasty wound. Once in the wound Cutibacterium can adhere to the prosthetic implants forming a biofilm that is resistant to host defenses and antibiotic treatment (see Cutibacterium recovered from deep specimens at the time of revision shoulder arthroplasty samples has increased biofilm-forming capacity and hemolytic activity compared with Cutibacterium skin isolates from normal subjects and Characterizing the Propionibacterium Load in Revision Shoulder Arthroplasty: A Study of 137 Culture-Positive Cases and Culturing explants for Cutibacterium at revision shoulder arthroplasty: an analysis of explant and tissue samples at corresponding anatomic sites.)
The diagnosis of Cutibacterium PJI of the shoulder is often not made until multiple cultures are obtained at revision surgery performed for pain, stiffness or component loosening. Making the diagnosis of Cutibacterium PJI before revision surgery is complicated by two facts: (1) the clinical presentation of these infections is frequently subtle, frequently without the typical symptoms, signs, and laboratory evidence of infection (fever, swelling, tenderness, erythema, elevated white blood cell counts, erythrocyte sedimentation rate, C reactive protein, serum inflammatory markers and positive joint aspirates) (see Propionibacterium in Shoulder Arthroplasty: What We Think We Know Today) and (2) the clinical onset of Cutibacterium can be delayed by months or years after the index procedure (see Substantial cultures of Propionibacterium can be found in apparently aseptic shoulders revised three years or more after the index arthroplasty.).
Because the causative organism is different, the risk factors for shoulder PJI are quite different than those for hip and knee PJI. Cutibacterium PJI is more common among young, male patients in good overall health as indicated by American Society of Anesthesiologists class I, with high levels of Cutibacterium on cultures of swabs of the unprepared shoulder skin surface, and elevated serum testosterone levels (either from endogenous causes or because of testosterone supplements)(see Preoperative Skin-Surface Cultures Can Help to Predict the Presence of Propionibacterium in Shoulder Arthroplasty Wounds and Preoperative skin cultures are predictive of Propionibacterium load in deep cultures obtained at revision shoulder arthroplasty and Preoperative Skin Cultures Predict Periprosthetic Infections in Revised Shoulder Arthroplasties: A Preliminary Report and Factors predictive of Cutibacterium periprosthetic shoulder infections: a retrospective study of 342 prosthetic revisions and Association Between Serum Testosterone Levels and Cutibacterium Skin Load in Patients Undergoing Elective Shoulder Arthroplasty: A Cohort Study.
While the effectiveness of prophylactic measures has yet to be rigorously demonstrated, patients at increased risk may benefit from extraordinary measures to reduce the chance of shoulder PJI, such as potent perioperative antibiotics (Ceftriaxone and Vancomycin), povidone-iodine washes of the surgical field, topical in wound antibiotics (such as Vancomycin), and a course of postoperative antibiotics (Doxycycline or Augmentin). Conversely, the cost and risks of these measures can be avoided in patients at low risk.
You can support cutting edge shoulder research that is leading to better care for patients with shoulder problems, click on this link.
Follow on twitter: https://twitter.com/shoulderarth
Follow on facebook: click on this link
Follow on facebook: https://www.facebook.com/frederick.matsen
Follow on LinkedIn: https://www.linkedin.com/in/rick-matsen-88b1a8133/
Here are some videos that are of shoulder interest
Shoulder arthritis - what you need to know (see this link).
How to x-ray the shoulder (see this link).
The ream and run procedure (see this link).
The total shoulder arthroplasty (see this link).
The cuff tear arthropathy arthroplasty (see this link).
The reverse total shoulder arthroplasty (see this link).
The smooth and move procedure for irreparable rotator cuff tears (see this link).
Shoulder rehabilitation exercises (see this link).
You can support cutting edge shoulder research that is leading to better care for patients with shoulder problems, click on this link.
Follow on twitter: https://twitter.com/shoulderarth
Follow on facebook: click on this link
Follow on facebook: https://www.facebook.com/frederick.matsen
Follow on LinkedIn: https://www.linkedin.com/in/rick-matsen-88b1a8133/
Here are some videos that are of shoulder interest
Shoulder arthritis - what you need to know (see this link).
How to x-ray the shoulder (see this link).
The ream and run procedure (see this link).
The total shoulder arthroplasty (see this link).
The cuff tear arthropathy arthroplasty (see this link).
The reverse total shoulder arthroplasty (see this link).
The smooth and move procedure for irreparable rotator cuff tears (see this link).
Shoulder rehabilitation exercises (see this link).
