In his classic paper, Morphologic study of the glenoid in primary glenohumeral osteoarthritis, Gilles Walch identified the B1 and B2 glenoids as being common of types of arthritic glenohumeral pathoanatomy in patients presenting for anatomic shoulder arthroplasty.
An important characteristic of these glenoid types is the posterior decentering of the humeral head on the glenoid, a critical element in the evaluation and management of glenohumeral arthritis. Note that the degree of decentering was (and remains) defined by the relationship of the humeral head to the face of the glenoid (and not the plane of the scapula), as seen from this figure from his classic article.
The decentering of the head on the glenoid can be evaluated on the standardized axillary "truth" view, as shown in the five examples below.
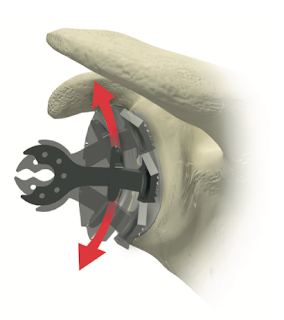
By the "truth" view, we mean an axillary view obtained with the arm elevated in the plane of the scapula that shows the spinoglenoid notch or "eye" (red arrow) as shown in this Steve Lippitt illustration:
The rationale for evaluating decentering with the arm elevated to a functional position is that CTs or MRIs obtained with the arm at the side may not reveal it, as shown in the two images of the same shoulder shown below. The MRI obtained with the arm at the side does not reveal decentering, whereas dramatic posterior decentering is shown when the arm is elevated to a functional position in the axillary "truth" view.
While often considered together, the B1 and B2 are not the same. The B1 has posterior decentering of the humerus on the glenoid without biconcavity of the glenoid from bony erosion. By contrast, the B2 has posterior decentering of the humeral head on the glenoid with biconcavity of the glenoid as shown in these illustrations from the classic article by Walch.
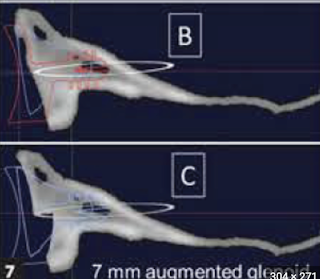
A third B was added by the authors of A modification to the Walch classification of the glenoid in primary glenohumeral osteoarthritis using three-dimensional imaging.
As can be seen from these figures, the B3 is monoconcave (i.e. no biconcavity) with substantial retroversion and without posterior decentering of the humeral head on the glenoid, i.e. the humeral head is centered with respect to the glenoid.
This point is emphasized by the authors of Quantitative measurement of bony pathology in advanced glenohumeral osteoarthritis who use the term "humeral-glenoid alignment (HGA)" to indicate centering or decentering of the humeral head on the glenoid. HGA is measured as the position of the humeral head center relative to the perpendicular line drawn from the glenoid center point (without reference to the scapular axis). This relationship is shown in a figure from their article showing the centering of the humeral head in a B3 glenoid (i.e. the humeral head is not decentered).
Follow on facebook: https://www.facebook.com/shoulder.arthritis
Follow on LinkedIn: https://www.linkedin.com/in/rick-matsen-88b1a8133/
Here are some videos that are of shoulder interest
Shoulder arthritis - what you need to know (see this link).
How to x-ray the shoulder (see this link).
The ream and run procedure (see this link)
The total shoulder arthroplasty (see this link)
The cuff tear arthropathy arthroplasty (see this link).
The reverse total shoulder arthroplasty (see this link).
The smooth and move procedure for irreparable rotator cuff tears (see this link)
Shoulder rehabilitation exercises (see this link).