While there is enthusiasm for the use of superior capsular reconstruction in the treatment of massive, irreparable cuff tears (see link, link, link, link) other reports have shown a bit more modest outcomes (see link, link, link, link, link, link, link,).
Thus, it is timely to consider three recent reviews of this procedure.
First: Superior Capsular Reconstruction Indications, Techniques, and Clinical Outcomes
"Despite its rapid growth in popularity and several biomechanical studies evaluating the technique, clinical outcome literature for superior capsular reconstruction remains limited to date."
Second: Superior Capsular Reconstruction for Massive Rotator Cuff Tears A Critical Analysis Review
"Arthroscopic superior capsular reconstruction with fascia lata autograft or humeral dermal allograft is a surgical option, with multiple studies showing statistically significant improvement in short-term outcomes for both pain and function among younger patients with massive irreparable rotator cuff tears. The long-term clinical effectiveness and value have yet to be determined."
"No comprehensive quality-of-life or cost-comparison analyses are available to compare superior capsular reconstruction, reverse total shoulder arthroplasty (rTSA), tendon transfer, and partial rotator cuff repair for the treatment of massive irreparable rotator cuff tears. However, the potential higher cost of superior capsular reconstruction and the lack of long-term clinical outcomes or revision data suggest that either an attempt at repair or primary arthroplasty may be more cost-effective than superior capsular reconstruction."
"Long-term outcome data are essential to determine the role of superior capsular reconstruction for young patients with massive irreparable rotator cuff tears."
"Superior capsular reconstruction using fascia lata autograft may provide a different biomechanical and biological healing environment compared to acellular dermal allograft. Thus, the clinical outcome data between the 2 graft methods should not be generalized."
Third: Outcome Comparison of Graft Bridging and Superior Capsule Reconstruction for Large to Massive Rotator Cuff Tears: A Systematic Review
A systematic review was performed via a comprehensive search of PubMed, Embase, and the Cochrane Library. Studies of Graft Bridging (GB) or Superior Capsular Reconstruction). Twenty-three studies were included in this review. Overall, both procedures demonstrated improvement of clinical outcomes. When compared with group SCR, group GB had significantly higher mean differences of the Constant-Murley score (41.9 vs 19.8), American Shoulder and Elbow Surgeons score (39.3 vs 33.8), visual analog scale score for pain (4.4 vs 3.4), and active external rotation at side (15.3 vs 9.3).
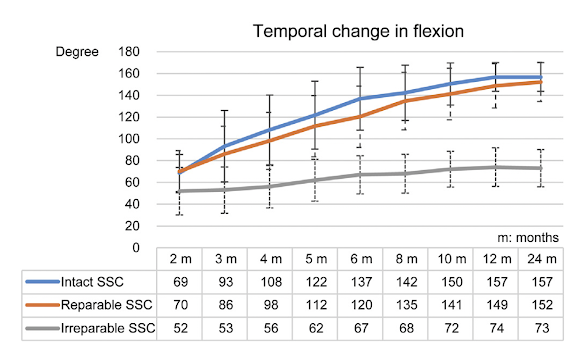
No statistically significant difference was detected in the mean difference of active forward flexion, internal rotation, abduction, and graft healing rate between the groups. The complication rates were 0.84% (2 of 238) in group SCR and 0.67% (4 of 593) in group GB.
These authors concluded that graft bridging showed significantly better clinical and functional outcomes postoperatively than SCR, with a similar complication rate. The available fair-quality evidence suggested that GB might be a better choice for large to massive RCT. More high-quality randomized controlled studies are required to further evaluate the relative benefits of the 2 procedures.
Comment: With respect to non-arthritic massive irreparable cuff tears, we recognize that the clinical presentation varies widely from minimal symptoms, to stiffness, to painful crepitance, to pseudoparalysis. Because these tears are usually chronic, a good try at rehab directed at optimizing passive and active motion is indicated (see link). It is impressive to see patients referred for a reverse total shoulder who are improved to the point of satisfaction by this approach. For patients with retained active elevation, a smooth and move procedure (see link) can provide improved comfort and function without the prolonged down time associated with soft tissue reconstruction or arthroplasty.
As can be seen from the reviews summarized above, the indications for, surgical technique and graft choice used, and the results of superior capsular reconstruction differ widely among authors.
We've much yet to learn about the treatment for the different symptoms associated with irreparable cuff tears.
Here are some videos that are of shoulder interest
Shoulder arthritis - what you need to know (see this link). How to x-ray the shoulder (see this link). The total shoulder arthroplasty (see this link). The ream and run technique is shown in this link. The cuff tear arthropathy arthroplasty (see this link). The reverse total shoulder arthroplasty (see this link). The smooth and move procedure for irreparable rotator cuff tears (see this link). Shoulder rehabilitation exercises (see this link).