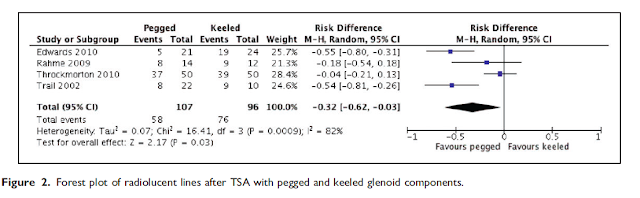
These authors conducted a systematic review of total shoulders to consider which fixation options provides optimal long-term functional outcomes with decreased rates of revision surgery and radiolucency. They found 7 comparative studies and 25 noncomparative studies were included in the final analysis, including 4 randomized (level I) studies, 1 level II study, 8 level III studies, and 19 level IV studies.
Meta-analysis of the comparative studies demonstrated a higher rate of revision surgery with keeled fixations compared with pegged fixations (odds ratio, 6.22; 95% confidence interval [CI], 1.38-28.1; P . .02).
They found that the differences with respect to functional outcomes, such as the American Shoulder and Elbow Surgeons score (mean difference, 9.54) and Constant score (mean difference 5.31), as well as radiolucency rates (odds ratio, 1.89) were present but not statistically significant with the number of included studies.
Comment: Such studies are confounded by the fact that "pegged" glenoids come in a wide variety of peg types and configurations, each of which may affect its clinical and radiographic durability. So that conclusions about the performance of a "pegged" glenoid with out considering the component design.
The Radiographic Evaluation of Keeled and Pegged Glenoid Component Insertion
Background: Radiolucent lines about the glenoid component of a total shoulder replacement are a common finding, even on initial postoperative radiographs. The achievement of complete osseous support of the compo- nent has been shown to decrease micromotion. We evaluated the ability of a group of experienced shoulder surgeons to achieve complete cementing and support in a series of patients managed with keeled and pegged glenoid components.
Methods: We reviewed the initial postoperative radiographs of 493 patients with primary osteoarthritis who had been managed with total shoulder arthroplasty by seventeen different surgeons. One hundred and sixty-five pa- tients were excluded because of inadequate radiographs, leaving 328 patients available for review. Of these, thirty-nine patients had a keeled component and 289 had a pegged component. The method of Franklin was used to grade the degree of radiolucency around the keeled components, and a modification of that method was used to grade the degree of radiolucency around the pegged components. The efficacy of component seat- ing on host subchondral bone was evaluated with a newly constructed five-grade scale based on the percentage of the component that was supported by subchondral bone. Each radiograph was graded four times, by two sep- arate reviewers on two separate occasions.
Results: Radiolucencies were extremely common, with only twenty of the 328 glenoids demonstrating no radi- olucencies. On a numeric scale (with 0 indicating no radiolucency and 5 indicating gross loosening), the mean radiolucency score was 1.8 ± 0.9 for keeled components and 1.3 ± 0.9 for pegged components (p = 0.0004). After defining categories of “better” and “worse” cementing, we found that pegged components more com- monly had “better cementing” than did keeled components (p = 0.0028). Incomplete seating was also com- mon, particularly among patients with keeled components. Ninety-five of the 121 pegged components that had been inserted by the most experienced surgeon had “better cementing,” compared with eighty-five of the 168 pegged components that had been inserted by the remaining surgeons (p < 0.00001).
Conclusions: Perfectly cementing and seating a glenoid replacement is a difficult task. Radiolucencies and in- complete component seating occur more frequently in association with keeled components compared with pegged components. Surgeon experience may be an important variable in the achievement of a good technical outcome.
====
Finally, it is important to recognize that glenoid component lucencies do, in fact have clinical consequences as shown in the article below.
Glenoid component lucencies are associated with poorer patient-reported outcomes following anatomic shoulder arthroplasty
Background
High rates of radiographic glenoid loosening following anatomic total shoulder arthroplasty (TSA) are documented at midterm follow-up. Small studies remain conflicted on the impact of lucent lines on clinical outcomes. This study assesses the impact of radiolucent lines on function and patient-reported outcomes (PROs) following TSA.
Methods
We retrospectively evaluated 492 primary TSAs performed between February 2005 and April 2016. Radiographs were evaluated for glenoid loosening according to the Lazarus grade at a mean of 5.3 years (range, 2-12 years). Clinical outcome measures included range of motion and American Shoulder and Elbow Surgeons, Constant, University of California–Los Angeles, Simple Shoulder Test, and Shoulder Pain and Disability Index scores. Outcomes were compared between patients with and patients without glenoid lucent lines and in relation to lucency grade.
Results
At most recent follow-up, 308 glenoids (63%) showed no radiolucent lines (group 0) and 184 demonstrated peri-glenoid lucencies (group 1). The groups were similar regarding age, sex, body mass index, comorbidities, and prior surgery. At follow-up, group 1 demonstrated significantly lower improvements in forward elevation (P = .02) and all PROs (P ≤ .005). Subgroup analysis by radiolucency grade showed that forward elevation diminished with increasing radiolucent score and exceeded the minimal clinically important difference (MCID) above grade 2 lucencies. A similar decline in PROs was observed with increasing lucency grade. These differences did not exceed the MCID below grade 5 lucencies.
Discussion
Peri-implant glenoid lucencies following TSA are associated with lower forward elevation and PROs. Lucencies above grade 2 are associated with clinically important losses in overhead motion. However, differences below the MCID are maintained for PROs below grade 5 glenoid lucencies.
====
In our experience, careful conservative carpentry of the glenoid bone to match the geometry of a glenoid component with a fluted central peg and optimal cementing technique leads to minimal issues with lucent lines or fixation failure. No cement is used on the backside of the glenoid component.
====
We have a new set of shoulder youtubes about the shoulder, check them out at this link.
Comment: Such studies are confounded by the fact that "pegged" glenoids come in a wide variety of peg types and configurations, each of which may affect its clinical and radiographic durability. So that conclusions about the performance of a "pegged" glenoid with out considering the component design.
Secondly, as is pointed out in the article below, studies of glenoid component durability are as much about the experience and technique of the surgeon as they are about component design.
The Radiographic Evaluation of Keeled and Pegged Glenoid Component Insertion
Background: Radiolucent lines about the glenoid component of a total shoulder replacement are a common finding, even on initial postoperative radiographs. The achievement of complete osseous support of the compo- nent has been shown to decrease micromotion. We evaluated the ability of a group of experienced shoulder surgeons to achieve complete cementing and support in a series of patients managed with keeled and pegged glenoid components.
Methods: We reviewed the initial postoperative radiographs of 493 patients with primary osteoarthritis who had been managed with total shoulder arthroplasty by seventeen different surgeons. One hundred and sixty-five pa- tients were excluded because of inadequate radiographs, leaving 328 patients available for review. Of these, thirty-nine patients had a keeled component and 289 had a pegged component. The method of Franklin was used to grade the degree of radiolucency around the keeled components, and a modification of that method was used to grade the degree of radiolucency around the pegged components. The efficacy of component seat- ing on host subchondral bone was evaluated with a newly constructed five-grade scale based on the percentage of the component that was supported by subchondral bone. Each radiograph was graded four times, by two sep- arate reviewers on two separate occasions.
Results: Radiolucencies were extremely common, with only twenty of the 328 glenoids demonstrating no radi- olucencies. On a numeric scale (with 0 indicating no radiolucency and 5 indicating gross loosening), the mean radiolucency score was 1.8 ± 0.9 for keeled components and 1.3 ± 0.9 for pegged components (p = 0.0004). After defining categories of “better” and “worse” cementing, we found that pegged components more com- monly had “better cementing” than did keeled components (p = 0.0028). Incomplete seating was also com- mon, particularly among patients with keeled components. Ninety-five of the 121 pegged components that had been inserted by the most experienced surgeon had “better cementing,” compared with eighty-five of the 168 pegged components that had been inserted by the remaining surgeons (p < 0.00001).
Conclusions: Perfectly cementing and seating a glenoid replacement is a difficult task. Radiolucencies and in- complete component seating occur more frequently in association with keeled components compared with pegged components. Surgeon experience may be an important variable in the achievement of a good technical outcome.
====
Finally, it is important to recognize that glenoid component lucencies do, in fact have clinical consequences as shown in the article below.
Glenoid component lucencies are associated with poorer patient-reported outcomes following anatomic shoulder arthroplasty
Background
High rates of radiographic glenoid loosening following anatomic total shoulder arthroplasty (TSA) are documented at midterm follow-up. Small studies remain conflicted on the impact of lucent lines on clinical outcomes. This study assesses the impact of radiolucent lines on function and patient-reported outcomes (PROs) following TSA.
Methods
We retrospectively evaluated 492 primary TSAs performed between February 2005 and April 2016. Radiographs were evaluated for glenoid loosening according to the Lazarus grade at a mean of 5.3 years (range, 2-12 years). Clinical outcome measures included range of motion and American Shoulder and Elbow Surgeons, Constant, University of California–Los Angeles, Simple Shoulder Test, and Shoulder Pain and Disability Index scores. Outcomes were compared between patients with and patients without glenoid lucent lines and in relation to lucency grade.
Results
At most recent follow-up, 308 glenoids (63%) showed no radiolucent lines (group 0) and 184 demonstrated peri-glenoid lucencies (group 1). The groups were similar regarding age, sex, body mass index, comorbidities, and prior surgery. At follow-up, group 1 demonstrated significantly lower improvements in forward elevation (P = .02) and all PROs (P ≤ .005). Subgroup analysis by radiolucency grade showed that forward elevation diminished with increasing radiolucent score and exceeded the minimal clinically important difference (MCID) above grade 2 lucencies. A similar decline in PROs was observed with increasing lucency grade. These differences did not exceed the MCID below grade 5 lucencies.
Discussion
Peri-implant glenoid lucencies following TSA are associated with lower forward elevation and PROs. Lucencies above grade 2 are associated with clinically important losses in overhead motion. However, differences below the MCID are maintained for PROs below grade 5 glenoid lucencies.
====
In our experience, careful conservative carpentry of the glenoid bone to match the geometry of a glenoid component with a fluted central peg and optimal cementing technique leads to minimal issues with lucent lines or fixation failure. No cement is used on the backside of the glenoid component.
====
We have a new set of shoulder youtubes about the shoulder, check them out at this link.
Be sure to visit "Ream and Run - the state of the art" regarding this radically conservative approach to shoulder arthritis at this link and this link
Use the "Search" box to the right to find other topics of interest to you.
You may be interested in some of our most visited web pages arthritis, total shoulder, ream and run, reverse total shoulder, CTA arthroplasty, and rotator cuff surgery as well as the 'ream and run essentials'