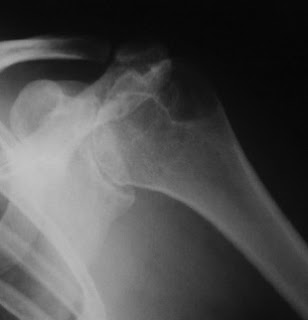
Surface replacement arthroplasty for glenohumeral arthropathy in patients aged younger than fifty years: results after a minimum ten-year follow-up
These authors present a case series of 54 cementless surface replacement arthroplasties (49 patients (25 men, 24 women)(average age 38.9 years (range, 22-50 years)) performed between 1990 and 2003. Of these, 38 patients (42 shoulders) were available for followup at a mean of 14.5 years (range, 10-25 years) after surgery.
17 were total shoulder replacements with metal back keeled glenoids, and 37 were humeral head resurfacing with microfracture of the glenoid.
It is of note that the diagnoses in this report from the UK were as follows:
avascular necrosis, 16
rheumatoid arthritis, 20
instability arthropathy, 7
primary osteoarthritis, 5
fracture sequelae, 3
postinfection arthritis, 2
psoriatic arthritis, 1
17 cases had full thickness cuff tears or poor quality rotator cuffs.
The deltopectoral approach was used in 20 shoulders and the anterosuperior (Neviaser-Mackenzie) approach in 34. The anterosuperior approach became the preferred approach in1993.
The mean relative Constant score increased from 11.5% to 71.8%, the results with humeral head resurfacing with microfracture of the glenoid (77.7%) were superior to those with total resurfacing arthroplasty that included a glenoid component (58.1%).
The best results were observed for the AVN patients, with Constant score improving from 13% to 85%. These were followed by the primary osteoarthritis group results and the rheumatoid arthritis group which had more modest results but high levels of satisfaction.
In 35 of 38 shoulders the humeral implants showed no lucencies. All of the humeral lucencies were observed in cases having a glenoid component. There were 9 glenoid implants of which 4 were loose.
15 had severe superior migration, 5 had moderate superior migration, and 2 had mild superior migration. 16 shoulders showed no superior migration.
Moderate to severe glenoid erosion was present in 12 of the shoulders at an average follow-up of more than 14.5 years. Glenoid erosion was correlated with superior migration of the humeral head and was more prevalent in patients with rheumatoid arthritis.
The mean time from the index arthroplasty to the revision surgery was 12 years
2 shoulders required early arthrodesis due to instability and deep infection.
In addition, 10 of 54 shoulders required revision arthroplasty.
The indications for revision arthroplasty were rotator cuff failure in 4 shoulders (3 HSA and 1 TSA), glenoid loosening and humeral loosening in 4 TSA shoulders, glenoid erosion in 1 HSA
shoulder, and 1 traumatic periprosthetic fracture.
7 were revised to stemmed prosthesis: 1 for traumatic fracture and 1 for glenoid erosion 16 years after the index procedure.5 shoulders in 4 patients (4 rheumatoid arthritis, 1 avascular necrosis) were revised at 8 to 14 years after surgery for cuff failure and loosening.
3 were revised to stemless reverse total shoulder arthroplasty due to rotator cuff failure at 23, 16, and 13 years after surgery.
Comment: This is an interesting and candid report by authors that include the designer of this system. Firstly, all shoulder surgeons recognize that the <50 year old patient needing an arthroplasty provides special challenges due to expectations, activities, and relatively uncommon diagnoses. Secondly, the patients in this series had a high preoperative incidence of rotator cuff issues, which place arthroplasty at increased risk of failure. Thirdly, the high rate of glenoid component loosening (often accompanied by humeral component loosening) and low clinical scores in the total shoulder group may be in part due to the technical challenge of glenoid arthroplasty when a substantial amount of the humeral head bone is retained as in these resurfacing arthroplasties - a feature that may compromise exposure.
Points of interest include the use of microfracture, the fact that 7 of the 10 revision arthroplasty were from resurfacing to stemmed prostheses, and the use of arthrodesis for two of the failures.
All in all, this article provides an interesting contrast to our local practice and it will be of interest to see how all of us evolve in our management of the young, arthritic shoulder.
Use the "Search" box to the right to find other topics of interest to you.